Case Quiz (May 2016)
A 9-month-old girl, born to non-consanguineous parents, with normal antenatal ultrasound and no history of renal disease in the family was noticed to have occasional vomiting since birth. Gradually her vomiting increased associated with diarrhea at 4 months of life. On evaluation, she was found to have serum creatinine level of 3.3 mg/dL and potassium of 4.2 mEq/L. U/S showed left pelvic kidney and normally placed right kidney, which were of normal size with increased echogenecity and loss of corticomedullary differentiation. She was managed with IV fluids and peritoneal dialysis for 4 days at the local center. She improved symptomatically but had persistently elevated serum creatinine of 1.4-1.8 mg/dL.At 9 months, she weighed 5.25 kg, was anemic with no dysmorphic features. She was well hydrated but had acidotic breathing; blood pressure level was 80/60 mm Hg.Investigations showed serum creatinine of 2.0 mg/dL, sodium 143 mEq/L, potassium 4.6 mEq/L, chloride 115 mEq/L, bicarbonate11 mEq/L, total protein 7.9 g/dL, albumin 3.9 g/dL, cholesterol 334 mg/dL, calcium 9.0 mg/dL, phosphorus 2.7 mg/dL, alkaline phosphatase 1583 IU/L, uric acid 13 mg/dL, hemoglobin 6.1 g/dL and PCV 17%. Urinalysis showed specific gravity of 1.010, pH 5.0, albumin 3+ and occasional RBCs. The random urine protein was 397 mg/dL and creatinine 10 mg/dL; protein to creatinine ratio 39.7. U/S examination confirmed the previous findings. Micturating crystourethrogram showed no evidence of VUR.The patient was managed with oral sodium bicarbonate (5 mL three times a day) and oral allopurinol (25 mg twice a day). She received packed cell transfusion, followed by subcutaneous injections of erythropoietin (250 IU weekly), oral iron (5 mg/kg/day) and folic acid (2.5 mg/day). An ultrasound guided renal biopsy was done on the right kidney under general anesthesia. I/F examination showed insignificant deposits of IgM and C3c in the glomeruli.
Case Answer (May 2016)
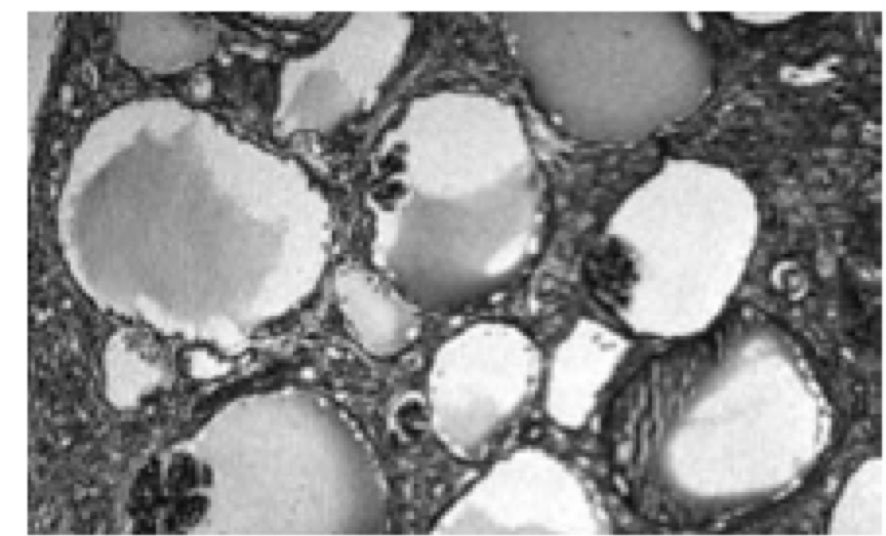
Glomerulocystic kidney disease (GCKD) is a rare renal cystic disease characterized by glomerular cysts (limited to renal cortex and > 5% cystic glomeruli) and may be associated with renal dysplasia and renal failure in infancy.
The presentation of GCKD varies, infants may present with an abdominal mass or renal insufficiency. In later childhood, the presentation may be with hematuria, proteinuria or abdominal pain. In cases of syndromic GCKD, patients are likely to present with other features. UTI may precede diagnosis of GCKD in obstructive causes.
In our case, the patient presented by renal insufficiency after an attack of gastro-enteritis. Loss of corticomedullary differentiation at the onset of the disease was not explained by gastro-enteritis. The patient developed, later on, proteinuria of glomerular origin in addition to other features of renal insufficiency. Biopsy was diagnostic.
Types of GCKD:
Type I: GCKD with early onset ADPKD.
Type II: Hereditary GCKD (AD) due to UMOD mutations or HNF1 mutations (familial hypoplastic GCKD).
Type III: Syndromic GCKD (e.g. tuberous sclerosis, Zellweger syndrome, Von Hipple Lindau disease and X-linked oral-facial-digital syndrome type I).
Type IV: Obstructive GCKD.
Type V: Sporadic GCKD